Click here for Frequently Asked Questions on Thyroid Nodules.
Thyroid nodules are common and are often detected incidentally when a patient has a neck ultrasound. A nodule may range in size from several mm to several cm, and may be detected visibly, by examination of the neck clinically, or by ultrasound assessment. Given the increasing availability of ultrasounds and frequency with which ultrasounds are obtained, incidental thyroid nodules are frequently first ascertained following ultrasound assessment. Small thyroid nodules detected only on ultrasound, generally only a few millimeters (mms) in size, are usually of minimal clinical significance. The majority of larger thyroid nodules are also benign, and usually do not produce symptoms.
Nevertheless, it is increasingly common for patients to have a thyroid nodule detected "incidentally" as part of an investigation for symptoms in the neck region that ultimately lead to a neck ultrasound and the detection of a thyroid nodule. Surprisingly, the risk of thyroid cancer in such small "incidentalomas" is still about 15-25%, as outlined in Prevalence, clinical and ultrasonographic characteristics of thyroid incidentalomas. Thyroid. 2004 Jan;14(1):29-33.
Most thyroid specialists advocate follow-up of incidentally detected thyroid nodules, sometimes with an initial biopsy, but an aggressive initial diagnostic approach with biopsy is not always indicated for small incidentally discovered nodules. See Thyroid incidentalomas. Prevalence, diagnosis, significance, and management. Endocrinol Metab Clin North Am. 2000 Mar;29(1):187-203. Thyroid nodules are managed similarly in a pediatric population, as outlined by published guidelines from the American Thyroid Association Management Guidelines for Children with Thyroid Nodules and Differentiated Thyroid Cancer The AmericanThyroid Association Guidelines Task Force on Pediatric Thyroid Cancer Thyroid. 2015 Apr 21.
There rare many diverse opinions amongst thyroid specialists with respect to the minimum size of a nodule that must be biopsied, with some specialists advocating biopsy of nodules greater than 1 cm in size, whereas others advocate biopsy of nodules greater than 1.5 cm in size. There are multiple factors that influence this decision, which should be discussed with your physician. For one approach, see Nonpalpable thyroid carcinoma: clinical controversies on preoperative selection. Am J Clin Oncol. 2003 Jun;26(3):232-5. To review guidelines suggested by the American Association of Clinical Endocrinologists, see American Association of Clinical Endocrinologists and Associazione Medici Endocrinologi medical guidelines for clinical practice for the diagnosis and management of thyroid nodules. Endocr Pract. 2006 Jan-Feb;12(1):63-102
Analysis of 1181 patients with one or more thyroid nodules > 10 mm in size revealed a diagnosis of thyroid cancer in 14.8% of patients (86% papillary thyroid cancer), with solitary nodules slightly more likely to be cancers versus than glands with multiple nodules. Cystic lesions were less likely than solid nodules to represent thyroid cancers, however the size of the nodule did not influence the likelihood of a malignant lesion. See Prevalence and distribution of carcinoma in patients with solitary and multiple thyroid nodules on sonography. J Clin Endocrinol Metab. 2006 Sep;91(9):3411-7. The incidence of thyroid cancer is somewhat higher, ~20%, in children with thyoid nodules FullA Standardized Assessment of Thyroid Nodules in Children Confirms Higher Cancer Prevalence than in Adults J Clin Endocrinol Metab. 2013 Jun 4.
As all patients are different, is not possible to make global recommendations about the diagnostic approach to thyroid nodules based on size alone. For example, in patients with other lumps or lymph nodes in the neck, a family history of thyroid cancer, or a history of irradiation, a more aggressive diagnostic work-up of a small nodule may be indicated. In other patients with very small incidental thyroid nodules who are healthy and without any unusual physical findings or associated risk factors, a more conservative initial diagnostic work-up and follow-up plan may be indicated. The decision as to how a thyroid nodule should be investigated depends on the clinical circumstances and should be discussed with your physician.
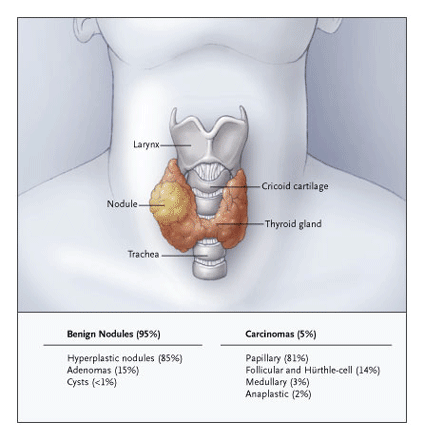
Nodules may be solid or filled with fluid (cystic). Thyroid cysts are less likely to be malignant, although cystic nodules with significant solid components (referred to as complex nodules) should be evaluated as solid nodules. Generally, the larger the nodule, the greater possibility that thyroid cancer may be present. Nevertheless, more than 90% of solid thyroid nodules are usually benign. Nodules may occur as single isolated occurrences (single or solitary nodules), or several nodules may be present (a multinodular gland). Having more than one nodule in the thyroid does not imply a more worrisome problem.
Nodules may also be classified as Functioning nodules (or Hot Nodules) or as Non-functioning (or cold), based on the results of radionucliide imaging studies (thyroid scans). Hot nodules are almost always benign (more than 95% of the time) and usually do not need to be investigated with needle biopsies unless they exhibit abnormal features and/or large size. If thyroid hormone production by hot nodules is excessive, this may lead to hyperthyroidism. Functioning nodules often arise as a consequence of changes or mutations in specific genes important for control of thyroid cell function and cell growth. These mutations are 'somatic mutations' that arise in the nodule only, but not every cell in the body and hence and are not usually hereditary. Recent studies indicate that the majority of hot nodules contain activating mutations in the TSH receptor gene. Mutations in genes that are directly coupled to control of thyroid cell cAMP, an intracellular second messenger that regulates growth, have also been identified. For an overview of genetic mutations in thyroid nodules, see J Clin Endocrinol Metab 1999 Nov;84(11):4155-8 Functioning and nonfunctioning thyroid adenomas involve different molecular pathogenetic mechanisms.
Although the majority of Cold nodules are also benign, cold nodules are more commonly monitored to make sure they do not represent thyroid cancers. Similarly, patients who have symptoms suggestive of compression in the neck, such as pain, difficulty with swallowing or breathing, or change in voice, or patients with swollen neck glands or lymph nodes should also be carefully investigated to rule out the presence of thyroid cancer. Patients who have significant cystic components to their nodule will have nodules that are partly 'cold' on scan, since the isotope will not be taken up by the cyst fluid. Although the mechanisms responsible for decreased iodine uptake in cold nodules have not been completely elucidated, the thyroid cells within the cold nodule appear to exhibit reduced expression or abnormal localization of the iodine transporter protein responsible for iodine uptake within thyroid cells. See Benign nonfunctioning thyroid adenomas are characterized by a defective targeting to cell membrane or a reduced expression of the sodium iodide symporter protein. J Clin Endocrinol Metab. 2002 Jan;87(1):352-7.
The size threshold for investigation of thyroid nodules using needle biopsy varies in different centers, with many clinicians electing to investigate and biopsy nodules from 1-2 cm in size and larger. Nevertheless, the decision to carry out needle biopsy depends on the history, examination, age of the patient, coexistent illnesses, other physical findings, and occasionally, associated ultrasound findings such as the pattern of calcification. Accordingly, size alone is not an absolute indicator of whether a biopsy needs to be carried out. In some instances, it may also be prudent to biopsy nodules smaller than 1 cm in size. In a study of small thyroid nodules picked up incidentally that were difficult to feel on examination, the risk of cancer in these nodules, 8-15 mm in size, was about 7-9%. In contrast, a second study of larger nodules detected by ultrasound that were difficult to feel revealed a much lower rate of cancer diagnosis after investigation with biopsies. Abnormal appearance of the nodules on ultrasound may help predict which nodules are more likely to be abnormal. Hence, the decision about how aggressive to be in the investigation of such nodules should individualized for each patient. See Risk of malignancy in nonpalpable thyroid nodules: predictive value of ultrasound and color-Doppler features. J Clin Endocrinol Metab. 2002 May;87(5):1941-6. and Clinical relevance of non-palpable thyroid nodules as assessed by ultrasound-guided fine needle aspiration biopsy. Endocrinol Invest. 2003 Jan;26(1):61-4 and Thyroid cancer in the thyroid nodules evaluated by ultrasonography and fine-needle aspiration cytology. Thyroid. 2005 Jul;15 (7): 708-17.
It is very unusual (not impossible) for small nodules to produce significant symptoms such as choking, voice problems, or trouble swallowing. If these symptoms are persistently present, a search for other causes, and a consultation with an ENT specialist, should be considered. Although common sense might predict that the size of the nodule corelates directly with the risk of cancer, once a nodule reaches 2 cm in size, the risk of thyroid cancer does not seem to increase much further, with relative cancer risks appearing similar in nodules that are 3 or 4 cm in size. Thyroid Nodule Size and Prediction of Cancer J Clin Endocrinol Metab. 2012 Dec 28
Diagnosis
Once a thyroid nodule has been detected, the thyroid hormone status (function of the thyroid) should be ascertained with a TSH. If the TSH is normal or modestly elevated, a Biopsy may be considered, contingent on the size of the nodule, whether it is solid or cystic, and depending on the presence of the associated features reviewed above. Some endocrinologists elect to carry out a thyroid scan first to see if a nodule is hypofunctioning or cold. Many endocrinologists will proceed straight to biopsy without a scan if the clinical scenario warrants this investigation. If an ultrasound has not been done, this may also be done at some point to assess precise nodule size, to determine whether the nodule is solid or cystic, or to look for other nodules or lymph nodes. If the TSH is abnormally low or undetectable, this raises the possibility that the nodule may be a "hot" or functioning nodule, which should prompt investigation with a thyroid scan, and occasionally, an iodine uptake (see Hot Nodule).
Treatment
The options for treatment of a patient with nodular thyroid disease range from periodic observation alone, to institution of thyroxine therapy and observation, to surgical excision. Patients with a Hot Nodule may also be candidates for radioactive iodine therapy.
Management should be tailored to the individual patient and the clinical scenario. The frequency of follow-up depends on the initial presentation, size of the nodule, associated symptoms, and biopsy results. Periodic ultrasounds may also be useful for precise quantification of nodule size and growth. As thyroid nodules are generally very slow growing, it is usually not necessary to repeat ultrasounds as frequently as every few months, except in rare circumstances.
The rationale for choosing to take thyroid hormone to suppress nodule growth is based on the observation that lowering the level of TSH (thyroid stimulating hormone) produced by the pituitary may prevent further growth of the nodule in some but not all patients. In some instances, patients on thyroxine may actually experience a small reduction in nodule size, but this usually takes many months or more commonly, years. As other factors may affect thyroid growth independent of TSH, thyroxine suppression is not always effective in preventing further thyroid nodule enlargement. In fact whereas some studies show that 25-50 % of patients taking thyroid hormone will have shrinkage of thyroid nodules, other studies do not show major reduction of nodule size in patients on thyroxine. Nodules that continue to enlarge despite effective TSH suppression merit particularly careful follow-up and repeat diagnostic assessment. Many patients elect to have their thyroid nodules followed on an ongoing basis without taking thyroid hormone. Furthermore, in patients with initial TSH levels that are borderline low, institution of thyroxine may actually result in a hyperthyroid state, especially if the patient has an "autonomous" thyroid gland that does not shut off its function and production of thyroid hormone and continues to make thyroid hormone inappropriately despite L-thyroxine therapy.
Frequency of Follow-Up
The frequency with which a nodule needs to be monitored and reassessed depends on the clinical scenario, size of the nodule, ultrasound and biopsy results, and preferences of both the patient and the physician. For example, an incidental 7 mm thyroid nodule detected on ultrasound might, in many medical practices, be reassessed safely on an annual basis. In contrast, a new nodule that was 3-4 cm in size that was "not present" several months ago, might in some cases be reassessed several months later with repeat biopsy and ultrasound. Patients should discuss the plan for ongoing follow-up and monitoring with their physician.
The majority of thyroid nodules, when followed over time, will exhibit some degree of enlargement, with almost 90% of nodules enlarging by at least 15% or more after several years of follow-up. See Natural history of benign solid and cystic thyroid nodules. Ann Intern Med. 2003 Feb 18;138(4):315-8.
Copyright Massachusetts Medical Society 2005 All rights reserved Utiger, R.D. NEJM 2005; 352:2376-2378
FAQs
My friend had a 1 cm nodule removed immediately from her breast and it turned out to be cancer. Why is it ok just to watch my thyroid nodule and not remove it immediately?
The vast majority of thyroid nodules, generally over 90%, are benign. Furthermore, most types of thyroid cancer, especially the most common types such as well differentiated cancer (papillary and follicular cancer), grow very slowly, and do not usually spread rapidly to other parts of the body, but most often remain confined to the neck. Hence, after appropriate investigations, if there is no evidence for thyroid cancer, it is quite common to simply observe the nodule, with follow-up and re-investigation at periodic intervals. The frequency and type of follow-up may also be influenced in part by the comfort level of the patient with the initial results and management plan.
Do I need to have a thyroid scan as part of my initial assessment?
Some patients with thyroid nodules will have thyroid scans, whereas others will not. Routine initial assessment includes a history, focused physical examination, and blood tests to ascertain thyroid function. If the possibility of malignancy exists, a biopsy is frequently done on the initial visit. In many instances, a thyroid scan to determine whether the nodule is functioning (hot nodule) or non-functioning (cold nodule) may not always add much information to the initial assessment. For example, if an ultrasound shows a nodule to be 90% cystic, the scan will not provide much additional information as the nodule will be viewed as "cold" on scan. Alternatively, patients with a suppressed or borderline low TSH may benefit from having a scan to see if the nodule is functioning (hot nodule). Similarly, an abundance of follicular cells on cytology may also suggest the possibility of an adenoma, for which a scan may add some additional functional information.
How often do I need to have my thyroid nodule reassessed?
The frequency of ongoing follow-up depends on the size of the nodule, the history of how rapidly the nodule appeared, associated findings on ultrasound, and other relevant findings from the history and clinical assessment. Larger nodules that have appeared suddenly need to be followed more frequently than an incidental 6 mm nodule detected on ultrasound. The precise plan for follow-up will depend on information obtained from the history, physical, and results of both clinical and laboratory assessment.
I had radiation to my neck as a teenager-should my nodules be managed differently?
Exposure to X-Rays, often ionizing radiation used years ago to treat acne or warts or infections or a large thymus or miscellaneous skin conditions, increases the risk of developing both benign nodules and thyroid cancer. For patients with a history of radiation exposure, a regular follow-up plan is indicated and attention to surveillance of more than just the "biggest nodule" may be prudent, as the risk of cancer appears to be slightly increased if more than one nodule is present as described in Size, number, and distribution of thyroid nodules and the risk of malignancy in radiation-exposed patients who underwent surgery. J Clin Endocrinol Metab. 2008 Jun;93(6):2188-93.
Will my nodule go away by itself?
Most solid thyroid nodules generally will not shrink spontaneously and completely disappear. Patients with a hemorrhage into a thyroid nodule may commonly experience reduction in size of the expanded nodule once the hemorrhage resolves. Similarly, patients with a nodular variant of Hashimoto's disease may notice nodules gradually getting bigger or smaller. Nevertheless, the majority of solid nodules remain persistent and detectable for many years.
Will the biopsy itself cause the spread of cancer along the track of the needle?
Despite the performance of hundreds of thousands of biopsies, this theoretical possibility has not been convincingly reported in the literature.
If the biopsy is normal, does this eliminate the possibility of cancer?
The sensitivity (accuracy) of biopsies ranges in different centers, and is usually 80-90%, and sometimes higher. Hence, it is usually not possible to state with 100% certainty that a single "negative" biopsy rules out the possibility of thyroid cancer. Accordingly, patients should always have a clearly defined plan for follow-up arranged with their physician as part of their ongoing management for their thyroid nodule.
Why did my doctor not do a thyroid biopsy as part of my initial assessment for my nodule?
The answer depends on the size of the nodule, whether it is solid or cystic, the age and associated medical features of the patient, and whether it has appeared recently or been present for a long period of time. For example, a patient with several small (5-10 mm) nodules is at very low risk of thyroid cancer, and many physicians may choose to follow these nodules without a biopsy at initial assessment. Nevertheless, even patients with thyroid nodules smaller than 10 mm may have a 10-15% risk of a small thyroid cancer, and the decision whether or not to proceed to biopsy should be discussed on an individual basis. See Ultrasonography-guided fine-needle aspiration of thyroid incidentaloma: correlation with pathological findings. Clin Endocrinol (Oxf). 2004 Jan; 60(1): 21-8.
I had my nodule surgically removed. Should I take thyroid hormone to suppress or prevent growth of additional nodules?
The optimal answer to this question remains unclear. Clearly, if the TSH level is even slightly elevated above normal, taking thyroid hormone is indicated. If the TSH is normal, the benefit of taking life long thyroid hormone in this scenario has not been clearly proven in randomized studies. Similarly, if the TSH is borderline low, it may be inappropriate for patients with benign nodular thyroid disease to take thyroid hormone. Data from retrospective studies suggests that thyroid hormone suppression may not be very effective in preventing the development of new nodules in patients after surgery for nodule removal. See Postoperative suppressive therapy for thyroid adenomas Am Surg 2000 Aug;66(8):751-5 and Effects of Thyroid-Stimulating Hormone Suppression with Levothyroxine in Reducing the Volume of Solitary Thyroid Nodules and Improving Extranodular Nonpalpable Changes: A Randomized, Double-Blind, Placebo-Controlled Trial by the French Thyroid Research Group. J Clin Endocrinol Metab. 2002 Nov 1;87(11):4928-4934
For years we just watched my nodule and did nothing about it. Now my physician says I might have cancer and I should have surgery. Why the sudden change in management?
Factors that influence the decision to recommend surgery include the size of the nodule, the pattern of historical growth and change in size of the nodule with time, the presence of new symptoms, the relationship of the nodule to local structures in the neck such as the trachea (airway), and the results of thyroid biopsies. The rate fo growth over time may help distinguish between benign and malignant nodules, and faster growing nodules may be considered for repeat biopsy Differential Growth Rates of Benign versus Malignant Thyroid Nodules The Journal of Clinical Endocrinology & Metabolism, jc.2017-01832
If you are not certain why surgery has been recommended, discuss the decision and the underlying reason(s) for the recommendation with your physician.
My friend had a 9 mm thyroid nodule and was told not to worry, and it turned out to be an aggressive thyroid cancer that spread. Why should I not have my 8 mm nodule removed?
There are always exceptions to the rule that very small nodules are usually benign, and hence management needs to be individualized according to the clinical circumstances present that are unique in each patient. Nevertheless, patients are reminded that the vast majority of small nodules less than 1 cm are benign. If all nodules such as these were removed surgically, it is likely that the number of patients exposed to complications of surgery would be relatively high compared to the number of patients that actually benefited from aggressive intervention. Nevertheless, the data clearly shows that even patients with 8-9 mm nodules do have a 10-15% incidence of thyroid cancer if the diagnosis is pursued aggressively. See Ultrasonography-guided fine-needle aspiration of thyroid incidentaloma: correlation with pathological findings. Clin Endocrinol (Oxf). 2004 Jan; 60(1): 21-8.
I was told cysts of the thyroid are never cancers. Is this true?
Although simple cysts with very thin walls are much less likely to be cancers than solid nodules, complex cysts that are partly solid and partly cystic need to be evaluated as if they were solid nodules, as sometimes cancers can present with partial cystic degeneration within the nodule. Attempts at biopsy of the solid component of the wall of the cysts, often under ultrasound guidance, are sometimes helpful in this scenario. The risk of thyroid cancer in a predominantly cystic lesion is still about 20%, as outlined in Management of cystic or predominantly cystic thyroid nodules: the role of ultrasound-guided fine-needle aspiration biopsy. Thyroid. 2004 Jan;14(1):43-7.
Should I take thyroid hormone or iodine to prevent further growth of my nodule(s)?
For many years, patients with nodules were often advised to take thyroid hormone (thyroxine) indefinitely to shrink or prevent further nodule growth. Indeed, many studies show that most nodules, but not all, will exhibit some degree of size reduction after a year or so on thyroxine. However, the nodules do not usually go away, and the need for follow-up and occasional repeat biopsy remains the same. Furthermore, some studies (Slow growth of benign thyroid nodules after menopause: no need for long-term thyroxine suppressive therapy in post-menopausal women. J Endocrinol Invest. 2004 Jan;27(1):31-6) show that nodules may not increase in size, even in the absence of thyroxine. The advantages and disadvantages of thyroxine therapy for nodules should be discussed with a physician and may vary, depending on nodule size, the TSH, and other factors. Although many areas of the world are now "iodine sufficient' there is some evidence that a combination of iodine supplementation (150 ug per day of potassium iodide) plus L-thyroxine (starting at 75 ug per day and increasing to titrate TSH to 0.2-0.8) is more effective at reducing nodule size than either iodine or thyroxine alone over a one year period. Nevertheless, the reduction in size was modest, and whether this regimen has long term benefit remains uncertain. Reduction of thyroid nodule volume by levothyroxine and iodine alone and in combination: a randomized, placebo-controlled trial Reduction of thyroid nodule volume by levothyroxine and iodine alone and in combination: a randomized, placebo-controlled trial J Clin Endocrinol Metab. 2011 Sep;96(9):2786-95
I had a PET scan and a spot was detected in the region of my thyroid gland. Do I need to have this investigated?
PET scans detect tissue that is metabolically active, including thyroid cancers, benign hot nodules, or inflammation. Nevertheless, given the importance of making a correct diagnosis in these circumstances, it is prudent to have an ultrasound, and if a nodule is detected, a biopsy, of any lesion detected on a PET scan. See FDG-PET Detected Thyroid Incidentalomas: Need for Further Investigation? Ann Surg Oncol. 2006 Oct 6; [Epub ahead of print] and Diagnostic and Clinical Significance of F-18-FDG-PET/CT Thyroid Incidentalomas J Clin Endocrinol Metab. 2012 Aug 17.
I am worried that my thyroid nodule might actually be another cancer that has spread to the thyroid-is this possible?
Secondary spread of other cancers, most commonly from primary tumors arising from lung, esophagus, breast, or kidney, has been described, but is extremely rare, likely accounting for less than 1/1000 cases of thyroid cancer. See Metastases to the thyroid gland: prevalence, clinicopathological aspects and prognosis: a 10-year experience. Clin Endocrinol (Oxf). 2007 Apr;66(4):565-71
I have big lymph glands (nodes) is my neck but my thyroid nodule biopsy was normal-are the two related?
All of us have lymph nodes throughout our body, including the neck region. Common reasons for enlarged neck nodes include a cold, sore throat, or upper respiratory tract infection, recent dental work or infection or inflammation in the mouth, jaw, or sinus. Inflammation in the thyroid gland, including thyroiditis, may also be associated with increased size and numbers of neck nodes. In many instances, lymph nodes associated with cancer have a different shape and appearance. However, some patients with thyroid cancer may have enlarged lymph nodes that look normal, but may be a clue to the presence of an abnormality in the thyroid gland. Hence ongoing surveillance and periodic re-evaluation of diagnostic options in cases like this seems prudent Enlarged Benign-Appearing Cervical Lymph Nodes by Ultrasonography Are Associated with Increased Likelihood of Cancer Somewhere Within the Thyroid in Patients Undergoing Thyroid Nodule Evaluation Thyroid. 2010 Jul 8. [Epub ahead of print]
Can genetic testing provide additional useful information about whether a nodule should be removed?
This is a very active area of clinical investigation. Some research studies have shown that changes (mutations) in specific cancer-causing genes may be more common in nodules that are more likely to be malignant. However this is still an area where more research needs to be done to confirm findings and evaluate whether they can be incorporated into clinical practice. Surgical Results of Thyroid Nodules according to a Management Guideline Based on the BRAFV600E Mutation Status J Clin Endocrinol Metab. 2011 Jan 14. [Epub ahead of print]
Are there non-surgical ways to shrink nodules that produce compressive symptoms?
A number of different options may be considered, depending on the size, iodine avidity, and local clinical experience with emerging technologies. For some large nodules with reasonable iodine uptake, radioactive iodine administered alone, or in combination with recombinant TSH may be considered. Some centres have experience with injection of alcohol into nodules, to destroy tissue. Other investigators have used radiofrequency thermal ablation with some success Optimum first-line treatment technique for benign cystic thyroid nodules: ethanol ablation or radiofrequency ablation? AJR Am J Roentgenol. 2011 Feb;196(2):W210-4 and Thyroid Nodules Treated with Percutaneous Radiofrequency Thermal Ablation: A Comparative Study J Clin Endocrinol Metab. 2012 Sep 27. and
Comparison of the Effectiveness of Ethanol and Radiofrequency Ablation in the Treatment of Thyroid Nodules and Their Effects on Cosmetic Scoring J Invest Surg. 2020 Dec 28:1-6. doi: 10.1080/08941939.2020.1866716 Other centres have reported very good success using image guided lasers to reduce the volume f and symptoms from thyroid nodues Outcomes and Risk Factors for Complications of Laser Ablation for Thyroid Nodules. A Multicenter Study on 1531 Patients J Clin Endocrinol Metab. 2015 Aug 14:jc20151964.
These approaches need to be considered after a malgnancy has been ruled out, and many of the experimental approaches may not be available in all centres.