Periodic news items relevant to thyroid disease, including new research studies from medical and scientific literature.
March 2003
Estrogen and thyroid hormone are two of the most common "hormones" that women will think about during various stages of their life. Given the enormous attention paid to menopause in some segments of society, and the potential clinical significance of menopause for many women, it is very common to wonder whether menopause is also associated with significant changes in levels of thyroid hormones. Sowers and colleagues examined levels of TSH and a number of menopause related symptoms in women of diverse ethnic background. African American women had significantly lower mean TSH concentrations than Caucasian, Hispanic and Chinese women. Women with TSH values outside the range of 0.5-5.0 mIU/ml were more likely to report shorter or longer menstrual periods (P = 0.004 for both), but levels of circulating sex steroid hormones did not correlate with TSH concentrations. Hence, thyroid status was not associated with menopausal symptoms or signs in this study. See: Thyroid stimulating hormone (TSH) concentrations and menopausal status in women at the mid-life: SWAN. Clin Endocrinol (Oxf). 2003 Mar;58(3):340-7.January 2003
From time to time, studies will examine whether there appears to be any relationship between breast cancer and thyroid disease. Although some studies find weak positive associations, many studies are negative. A new survey of subjects aged 35-64 years enrolled in a population-based, case-control study of invasive breast cancer was carried out at five sites in the United States. In-person interviews were completed for 4575 women (cases) with breast cancer (2953 white and 1622 black) and 4682 control women (3021 white and 1661 black). Breast cancer risk was not associated with treatment for thyroid disorders as described in Do thyroid disorders increase the risk of breast cancer? Cancer Epidemiol Biomarkers Prev. 2002 Dec;11(12):1574-8. Similarly, the results of a major large previous study of the possible relationship between these two cancers in 194,798 women who were diagnosed with invasive breast carcinoma (exclusive of those with distant metastasis) between 1973 and 1993 found no increased risk of thyroid cancer in patients treated with or without radiotherapy. See Risk of thyroid carcinoma in a female population after radiotherapy for breast carcinoma. Cancer. 2001 Sep 15;92(6):1411-1418.
Some authorities have postulated that since both thyroid cancer and breast cancer result in more careful medical assessment and regular follow-up of patients, there may be an element of detection bias in some women who turn out to have both diseases. See Second primary breast and thyroid cancers (Israel).Cancer Causes Control. 2003 May;14(4):367-75.
December 2002
A study of 4649 subjects in Denmark examined the relationship between the prevalence of thyroid disorders and multiple associated variables. Tobacco smoking was associated with an increased prevalence of thyroid multinodularity. The authors hypothesize that smokers have higher levels of the chemical thiocyanate, a degradation product of cyanide in tobacco smoke, which may block iodine uptake by the thyroid, leading to stimulation of nodule formation. See High occurrence of thyroid multinodularity and low occurrence of subclinical hypothyroidism among tobacco smokers in a large population study. J Endocrinol. 2002 Dec;175(3):571-6.
April 2002
Canadian Cancer Society Epidemiology Statistics in an easy to use Web-based format. Examine the changing trends in thyroid cancer incidence by region, age, sex, or compare variables. See Cancer of the Thyroid, Both Sexes Combined, All Ages, 1998, as a way to start.
Hypothyroidism is known to be associated with impairment of cognitive (mental) function, particularly if the hypothyroidism is severe. A study of 628 women 65 years or older enrolled in the Women's Health and Aging Study, a community-based study of physically impaired women assessed the relationship between cognitive function and levels of thyroid hormones on study entry, and after 1, 2, and 3 years, using the Mini-Mental State Examination (MMSE). The women who were included in this study were not normal healthy older women, but were women who reported difficulty with at least one task in at least two of four domains of functioning including mobility/exercise tolerance, upper extremity activities, basic self-care, and higher functioning tasks of independent living. Although no association between T(4) and TSH level and cognitive function was noted at the start of the study, those women with the lowest levels of thyroid hormones had a twofold risk of cognitive decline, leading the authors to conclude that thyroid hormone levels may contribute to cognitive impairment in physically impaired women. This study does not prove a cause and effect relationship between thyroid status and cognitive impairment, but raises the question of whether even small changes of thyroid hormone level within the normal range may be important for cognitive function in some clinical settings. See Serum thyroxine level and cognitive decline in euthyroid older women. Neurology. 2002 Apr 9;58(7):1055-1061.
Following pregnancy, women are often tired, sleep-deprived, and in some instances, some degree of emotional lability or depression may be present. As transient thyroid dysfunction following birth is not uncommon (see Postpartum thyroiditis), some experts have wondered whether treating everyone with thyroid hormone after pregnancy may prevent the onset of depression or emotional difficulties in women at risk who may have undiagnosed thyroid problems. In a randomized double-blind placebo-controlled trial, thyroxine or placebo was given daily to 446 thyroid-antibody-positive women (342 of whom were compliant) from 6 weeks to 6 months post-partum, with assessment of their psychiatric and thyroid status at regular intervals. The study showed that treatment with thyroxine had no effect on the occurrence of depression. See Randomized trial of thyroxine to prevent postnatal depression in thyroid-antibody-positive women. Br J Psychiatry. 2002 Apr;180(4):327-330.
A mild degree of hypothyroidism is not uncommon, and subclinical hypothyroidism is generally defined as the presence of a normal Free T4, slightly elevated TSH, and the questionable presence or absence of symptoms that may not be related to thyroid function. The treatment of subclinical hypothyroidism remains controversial, with some experts advocating that all such patients should be treated with thyroxine, whereas other thyroid experts advocate a more individualized approach. A new small randomized study in 40 women examined metabolic parameters and psychological function in women treated with thyroid hormone or placebo for six months. No significant clinical benefit could be observed in the thyroxine-treated subjects. See A 6-month randomized trial of thyroxine treatment in women with mild subclinical hypothyroidism. Am J Med. 2002 Apr 1;112(5):348-54.
March 2002
How useful are current localization techniques for identification of parathyroid adenomas in patients with hyperparathyroidism (HPT)? The answer depend on the clinical setting and context. The aim of the decision making process is to provide guidance to the surgeon in deciding whether a focal approach to surgery on one side of the neck is appropriate, or whether both sides of the neck need to be explored to find the abnormal parathyroid gland(s). An experienced group of surgeons report that a minimal approach can be considered in a select group of patients that does not have familial primary HPT, secondary or tertiary disease, coexisting thyroid pathology, or an equivocal sestamibi scan preoperatively. Only patients with a positive single hot spot on sestamibi scan can be considered candidates for the minimal approach. Using this criteria only 64% of all patients with hyperparathyroidism are candidates for a minimally invasive approach. See Parathyroid Surgery: Separating Promise from Reality. J Clin Endocrinol Metab. 2002 Mar 1;87(3):1024-1029.
February 2002
Thyroid disease is common. Researchers at the Centers for Disease Control and Prevention (CDC) evaluated the status of thyroid function by examining the TSH and thyroid antibodies in more than 17,000 subjects of the National Health and Nutritional Survey of the U.S. population from 1988 to 1994. The subjects were over the age of 12 and represented the geographic and ethnic distribution of the U.S. population. Nearly five percent of Americans suffer from undiagnosed thyroid disease, with more than four percent experiencing hypothyroidism. Hypothyroidism was more prevalent in white and Mexican Americans than in blacks and hypothyroidism was more common in women and older Americans. To review the survey data, see Serum TSH, T(4), and thyroid antibodies in the United States population (1988 to 1994): National Health and Nutrition Examination Survey (NHANES III). J Clin Endocrinol Metab. 2002 Feb;87(2):489-99.
Patients commonly ask why they develop thyroid disease. Although many disorders have an autoimmune basis, and sometimes iodine deficiency or excess may be important, for the majority of patients, we don't have a good answer to explain why thyroid disease develops. New epidemiological data now demonstrates that a history of smoking in women is associated with a higher risk of developing thyroid disorders. See Smoking as a risk factor for Graves' disease, toxic nodular goiter, and autoimmune hypothyroidism. Thyroid. 2002 Jan;12(1):69-75. Review of the literature suggest that smoking cessation may also reduce the risk of developing some types of thyroid disease, especially Graves' Disease. See Smoking and thyroid disorders - a meta-analysis. Eur J Endocrinol. 2002 Feb;146 (2):153-61.
January 9 2002
The available evidence supports the importance of maintaining both maternal and neonatal thyroid function in the normal range, so as to optimize intellectual and cognitive development in the fetus. A new study examines the effect of neonatal hypothyroidism, its correction, and subsequent assessment of intelligence, neuropsychological functioning, memory, and achievement. The data clearly shows that early correction of neonatal hypothyroidism is associated with improved performance on several of the standardized tests employed in this study. See The Influence of Etiology and Treatment Factors on Intellectual Outcome in Congenital Hypothyroidism. J Dev Behav Pediatr. 2001 Dec;22(6):376-384.
December 20 2001
Breast and thyroid cancer are common cancers in women. Some studies have raised the possibility that women with either breast or thyroid cancer have an increased risk of developing the other type of cancer. Furthermore, treatment of breast cancer with external radiation may rarely affect the thyroid, whereas some degree of radioactive iodine uptake in breast tissue may possibly occur after treatment of patients with thyroid cancer. A new study has examined the relationship between these two cancers in 194,798 women who were diagnosed with invasive breast carcinoma (exclusive of those with distant metastasis) between 1973 and 1993. No increased risk of thyroid cancer was detected in patients treated with or without radiotherapy. See Risk of thyroid carcinoma in a female population after radiotherapy for breast carcinoma. Cancer. 2001 Sep 15;92(6):1411-1418.
December 4 2001
Increasing thyroid cancer incidence in Canada, 1970-1996: time trends and age-period-cohort effects.
The number of patients with thyroid cancer seems to be clearly increasing. This study examines age-specific incidence rates comparing 1970 to 1996, and finds that the rate of reported thyroid cancer has doubled over this time period, to 6.8 and 2.2 per 100 000 in 1994-96, among females and males respectively, largely represented by well differentiated papillary carcinoma of the thyroid. The reason for the increased incidence, perhaps due to enhanced detection of smaller earlier lesions, is not clear. See Increasing thyroid cancer incidence in Canada, 1970-1996: time trends and age-period-cohort effects. Br J Cancer. 2001 Nov;85(9):1335-9.
December 3 2001
The majority of patients with non-medullary thyroid cancer, including patients with well differentiated thyroid cancers (WDTC) such as papillary or follicular thyroid cancers, do not have a familial component to their disease, and usually do not pass on a markedly increased risk of cancer to their children. Nevertheless, a small percentage of even WDTC patients do appear to develop the disease as a result of an as yet unknown genetic predisposition. In a new study of 339 patients with non-medullary forms of thyroid cancer, about 5% of cases reported at least one first degree relative with thyroid cancer. The identity of the gene(s) that account for this risk remains unknown., See Increased risk for nonmedullary thyroid cancer in the first degree relatives of prevalent cases of nonmedullary thyroid cancer: a hospital-based study. J Clin Endocrinol Metab. 2001 Nov;86(11):5307-12. A second study examined the risk of hereditary cancer in 1283047 cancer patients listed in the Swedish Cancer Registry. Of the more common types of familiar tumors, thyroid cancer was reported to have a "familiar index" of 6.2 compared to control subjects and other cancers. Nevertheless, it is not possible to distinguish between genetic and environmental influences that contribute to cancer development from this type of study. See Analysis of hereditary component of cancer by use of a familial index by site. Lancet. 2001 Nov 17;358(9294):1696-8.
November 8 2001
Premature infants manifest a range of biochemical and endocrine abnormalities, including, in some cases, low levels of circulating thyroid hormones. Osborn has now reviewed all trials that examined the potential benefit of thyroid hormone supplementation in such infants. Although none of the trials are perfect and the number of subjects studied is small, the available evidence do not show significant benefits for babies treated with thyroxine. See Thyroid hormones for preventing neurodevelopmental impairment in preterm infants (Cochrane Review). Cochrane Database Syst Rev. 2001;4:CD001070.
October 25 2001
Thyroxine treatment in patients with symptoms of hypothyroidism but thyroid function tests within the reference range: a randomized double blind placebo controlled crossover trial.
The symptoms of hypothyroidism are common and non-specific, and overlap with symptoms found in a normal population without laboratory evidence for thyroid dysfunction. Many patients are disappointed when informed that their tests show no evidence for thyroid abnormalities. A fringe element of health practioners claims current blood tests are inaccurate and use ancillary measures including hair analyses and body temperature as measures of thyroid function. To determine whether patients with such symptoms yet normal thyroid blood tests might benefit from thyroid hormone replacement, Pollock and colleagues administered 100 ug of thyroxine or placebo to 25 patients for 6 weeks in a crossover randomized trial. Study measurements included a battery of measures that assessed cognitive function and psychological and physical wellbeing. The results of the study clearly showed no significant improvement in these endpoints, despite higher levels of circulating thyroid hormones in the thyroxine treated patients. To review the data, see Thyroxine treatment in patients with symptoms of hypothyroidism but thyroid function tests within the reference range: randomized double blind placebo controlled crossover trial. BMJ. 2001 Oct 20;323(7318):891-5.
October 17 2001
Patients with hypothyroidism often have elevated levels of cholesterol, and treating the hypothyroidism frequently results in some degree of improvement in lipid (cholesterol) levels. A new study examines the impact of correcting mild subclinical hypothyroidism in women. The subjects, women with a mean TSH of ~ 11.7 were treated with placebo or thyroxine for 48 weeks. A modest but significant reduction in total and LDL cholesterol was observed in the group receiving sufficient thyroxine to correct the TSH to normal. See TSH-controlled l-thyroxine therapy reduces cholesterol levels and clinical symptoms in subclinical hypothyroidism: a double blind, placebo-controlled trial (basel thyroid study). J Clin Endocrinol Metab. 2001 Oct;86(10):4860-6.
October 11 2001
Although a combination of whole body scanning after radioactive iodine AND measurement of circulating thyroglobulin represents an effective strategy for assessment of residual thyroid remnants and thyroid cancer in most patients, a small subset of patients have normal total body scans but elevated levels of thyroglobulin. After excluding assay-associated artifacts, the use of PET scans appears to result in considerably enhanced sensitivity for detection of residual thyroid cancer that may be below the threshold for detection by conventional 131-I scanning. It appears appropriate to recommend the use of PET scans for patients with unexplained increases in thyroglobulin with negative imaging studies using conventional radiological techniques. See Clinical impact of (18)f-fdg pet in thyroid carcinoma patients with elevated thyroglobulin levels and negative (131)i scanning results after therapy. J Nucl Med. 2001 Oct;42(10):1464-9.
October 3 2001
There is some evidence, from a small number of randomized trials, that patients with depression who receive treatment with a class of medications known as tricyclic antidepressants, will have a more favorable response if they are also treated with T3, the active form of thyroid hormone. The benefit, in some patients, appears to come in the form of a more rapid response to the anti-depressant medication, which can normally take 4-8 weeks to exert a beneficial therapeutic response. Not all the T3-treated patients show benefit, and the risks of T3 supplementation must be carefully assessed, versus the potential benefit in each patient. For more on this issue, see Optimal Thyroid Hormone Replacement. To review the recent Meta-Analysis that summarized data from the available randomized trials, see Does thyroid supplementation accelerate tricyclic antidepressant response? a review and meta-analysis of the literature. Am J Psychiatry. 2001 Oct;158(10):1617-22.
September 21 2001
A low TSH and excess cardiovascular mortality
What should the approach be to patients who are otherwise well, but have a low TSH indicative of biochemical, often "subclinical" hyperthyroidism. Clearly, the approach needs to be individualized for each patient. A population-based study examining the relationship between TSH and mortality found a small but significant increase in mortality from cardiovascular causes in 1191 persons not being actively treated with thyroxine or anti-thyroid medications. The results of this study do not prove treatment of the thyroid problem would reduce the risk of mortality, but they do provide further evidence linking hyperthyroidism to adverse cardiovascular (heart-related) events. Furthermore, if one has a suppressed TSH for another reason (hyperthyroidism, treatment of thyroid nodules, pituitary problems or thyroid cancer), there is no evidence suggesting that the TSH level correlates with increased mortality in these settings. Indeed, patients with thyroid cancer and a suppressed TSH exhibited a reduced risk of cancer-related mortality. For an overview of the relationship between cardiovascular problems and the heart, see Heart Disease.
The study Summary is reproduced below:
Prediction of all-cause and cardiovascular mortality in elderly people from one low serum thyrotropin result: a 10 year cohort study.
Lancet. 2001 Sep 15;358(9285):861-5
Background Low serum thyrotropin, in combination with normal concentrations of circulating thyroid hormones, is common, especially in elderly people and in individuals with a history of thyroid disease. We aimed to assess the long-term effects of subclinical hyperthyroidism on mortality. Methods We did a population-based study of mortality in a cohort of 1191 individuals not on thyroxine or antithyroid medication. All participants were aged 60 years or older. We measured concentration of thyrotropin in serum at baseline in 1988-89. We recorded vital status on June 1, 1999, and ascertained causes of death for those who had died. We compared data for causes of death with age-specific, sex-specific, and year-specific data for England and Wales. We also compared mortality within the cohort according to initial thyrotropin measurement. Results During 9733 person-years of follow-up, 509 of 1191 people died, the expected number of deaths being 496 (standardized mortality ratio [SMR] 1·0, 95% CI 0·9-1·1). Mortality from all causes was significantly increased at 2 (SMR 2·1), 3 (2·1), 4 (1·7), and 5 (1·8) years after first measurement in those with low serum thyrotropin (n471). These increases were largely accounted for by significant increases in mortality due to circulatory diseases (SMR 2·1, 2·2, 1·9, 2·0, at years 2, 3, 4, and 5 respectively). Increases in mortality from all causes in years 2-5 were higher in patients with low serum thyrotropin than in the rest of the cohort (hazard ratios for years 2, 3, 4, and 5 were 2·1, 2·2, 1·8, and 1·8, respectively). This result reflects an increase in mortality from circulatory diseases (hazard ratios at years 2, 3, 4, and 5 were 2·3, 2·6, 2·3, 2·3), and specifically from cardiovascular diseases (hazard ratios at years 2, 3, 4, and 5 were 3·3, 3·0, 2·3, 2·2). Interpretation A single measurement of low serum thyrotropin in individuals aged 60 years or older is associated with increased mortality from all causes, and in particular mortality due to circulatory and cardiovascular diseases.
September 6 2001
Patients and physicians are very aware that the symptoms of both hypothyroidism and hyperthyroidism are quite non-specific, and common in the general population frequently without biochemical confirmation of actual thyroid disease. This lack of correlation between symptoms and the presence of thyroid disease is often frustrating for all parties involved, leading some patients to question the validity and accuracy of thyroid hormone testing. A new study of this issue examined the presence or absence of symptoms and biochemical parameters of thyroid dysfunction in Danish subjects. Not surprisingly, the correlation between specific symptoms, and biochemical and clinical evidence for thyroid dysfunction was poor. To review the data, see Validity of self-reported hyperthyroidism and hypothyroidism: comparison of self-reported questionnaire data with medical record review. Thyroid. 2001 Aug;11(8):769-73.
September 1 2001
What is the status of minimally invasive approaches to thyroid surgery?
Although experience with this technique is still limited, the number of centers gaining experience with newer approaches to removal of thyroid nodules is increasing. See Minimally invasive video-assisted thyroidectomy. Am J Surg. 2001 Jun;181(6):567-70. for a description of the experience of a group of Italian physicians with video-guided minimally invasive surgery. For a related report, see Minimally invasive open thyroidectomy. Surg Today. 2001;31(8):665-9.
What is the current status of the Synthroid issue and FDA Guidelines? See Synthroid and the FDA.
August 15 2001
Menopause and thyroid cancer treatment
Radioactive iodine administration in high doses, as used in patients with thyroid cancer, is known to produce irregular menses for up to several months in ~25% of women, due to the effects on the ovaries. A retrospective analysis of 130 women treated with radioactive iodine prior to the age of 45 has demonstrated a slight but significant difference in the mean age of menopause onset (defined as lack of menstrual bleeding for 6 consecutive months). 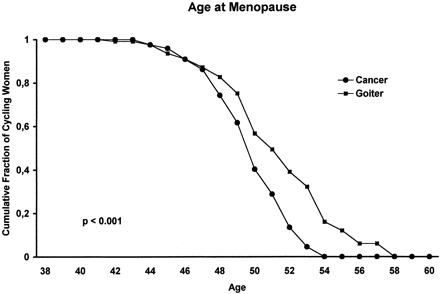 No significant difference in menopausal age was observed within the cancer group when this was subdivided according to 1) the age at initial treatment (less or more than 40 yr), 2) the age at the time of administration of the last 131I therapeutic dose (less or more than 45 yr), 3) the number of 131I administrations (one or repeated doses), and 4) cumulated dose (less or more than 3700 MBq). There was no evidence for impairment of fertility in this retrospective study. See 131I Therapy for Differentiated Thyroid Cancer Leads to an Earlier Onset of Menopause: Results of a Retrospective Study. J Clin Endocrinol Metab. 2001 Aug;86(8):3512-5
No significant difference in menopausal age was observed within the cancer group when this was subdivided according to 1) the age at initial treatment (less or more than 40 yr), 2) the age at the time of administration of the last 131I therapeutic dose (less or more than 45 yr), 3) the number of 131I administrations (one or repeated doses), and 4) cumulated dose (less or more than 3700 MBq). There was no evidence for impairment of fertility in this retrospective study. See 131I Therapy for Differentiated Thyroid Cancer Leads to an Earlier Onset of Menopause: Results of a Retrospective Study. J Clin Endocrinol Metab. 2001 Aug;86(8):3512-5
Role of PET scanning in the diagnosis and follow-up of thyroid cancer:
Many recent studies have advocated a potential role for the use of PET (positron emission tomography) scanning for detection of thyroid cancer. A review of research studies has concluded that most analyses of PET scans have been small making it difficult to draw widespread conclusions Diagnostic Accuracy of 18F-Fluorodeoxyglucose Positron Emission Tomography in the Follow-Up of Papillary or Follicular Thyroid Cancer.
J Clin Endocrinol Metab. 2001 Aug 1;86(8):3779-3786.
July 15 2001
Breast cancer and thyroid cancer are common tumors arising in women. Small studies have suggested a possible association between the two diseases in individual patients. The National Cancer Institute's Surveillance, Epidemiology and End Results (SEER) database, covering ~14% of the US population from 1973-1994 was used to examine the relative risks of developing both diseases in women. The results of the epidemiological analysis shows a small but significant increased relative risk of developing breast cancer following the diagnosis of thyroid cancer, with the risk most evident in white premenopausal women. These findings do not tell us why this relative risk might exist (environment versus genetics versus treatment effects etc). See The development of breast carcinoma in women with thyroid carcinoma. Cancer. 2001 Jul 15;92(2):225-31.
June 7 2001
Increased requirement for thyroid hormone in hypothyroid women receiving estrogen
Pregnancy is associated with a need to increase the dose of thyroxine in some women with hypothyroidism. A study of 11 postmenopausal women with normal thyroid function and 25 postmenopausal women with hypothyroidism demonstrated small, but potentially significant decreases in circulating levels of thyroxine, and increases in TSH, in some women with hypothyroidism. These findings suggest that free thyroid hormone and TSH levels should be reassessed following the start of estrogen therapy to determine adequacy of thyroid replacement in women with pre-existing hypothyroidism. Similarly, women with a history of thyroid cancer and thyroid surgery should have their TSH reassessed several months (12 weeks) after starting estrogen therapy. In contrast, patients taking thyroid hormone for "suppressive therapy" to prevent growth of nodules or goiters are not likely to need a change in thyroxine dose. See the study in the June 7 2001 issue of the New England Journal of Medicine.
May 2001
How accurate is health care information on the Internet? An independent assessment of this issue published in JAMA this May 2001assessed utility and accuracy of Search Engines for finding information, accuracy of information on various sites, and highlights pitfalls for consumers when assessing health-related information. In general, much of the information is accurate, but a high degree of reading comprehension is required. Review the study: Health Information on the Internet Accessibility, Quality, and Readability in English and Spanish JAMA. 2001;285:2612-2621.
May 2001
Cognitive Function and brain electrical function
What are the short and long term effects of L-thyroxine therapy that produces subclinical hyperthyroidism, as may be seen in patients taking thyroxine for thyroid cancer, on central nervous system function? Although there are few good studies of long term effects of excess L-thyroxine that are prospective and randomized, an intriguing short term double blind cross-over study in healthy young men demonstrates subtle but detectable effects of L-thyroxine, 0.3 mg daily for 3 weeks on several aspects of cognitive function and electrical brain activity. See Alterations of cognitive functions induced by exogenous application of thyroid hormones in healthy men: a double-blind cross-over study using event-related brain potentials. Thyroid. 2001 Apr;11(4):385-91.
April 2001
Risk for Fracture in Women with Low Serum Levels of Thyroid-Stimulating Hormone
Hyperthyroidism is known to be an independent risk factor for osteoporosis. Patients with hyperthyroidism who are treated generally experience an increase in bone mass following resolution of the hyperthyroidism. A prospective study of 686 women over the age of 65 found that hyperthyroidism, as detected using the TSH assay, was an independent risk factor for fracture risk. Importantly, women taking thyroid hormone with levels of TSH in the normal range did not have an increased risk of hip fracture. These findings emphasize the importance of monitoring TSH levels in patients on thyroid hormone replacement. Unless the patient has thyroid cancer, it seems prudent to avoid excess levels of thyroid hormone in similar patient populations. See Risk for Fracture in Women with Low Serum Levels of Thyroid-Stimulating Hormone Annals of Int Med 3 April 2001 Volume 134 Number 7.
March 2001
Should you take your L-thyroxine pills to the Antarctic?
Numerous changes in the endocrine system occur in response to changes in temperature, light cycles, and activity. Reed and colleagues have now studied a variety of parameters, including cognition, mood, depression, and exercise performance, both on and off exogenous thyroid hormone supplementation in 12 individuals working in the Antarctic. For most of the parameters studied, no major differences were seen on or off thyroxine. Slight but significant improvements in cognition were detected in the thyroxine-treated arm of the study. To review the data, see Impairment in Cognitive and Exercise Performance during Prolonged Antarctic Residence: Effect of Thyroxine Supplementation in the Polar Triiodothyronine Syndrome. J Clin Endocrinol Metab. 2001 Jan 1;86(1):110-116. New data on occupational radiation exposure and the risk of developing thyroid cancer. A longitudinal study of Canadian workers exposed with occupational radiation exposure clearly demonstrates an excess risk of thyroid cancer in study subjects, consistent with the known sensitivity of the thyroid gland to radiation-induced mutations. To review the data for all Cancers and for thyroid disease, see First Analysis of Cancer Incidence and Occupational Radiation Exposure Based on the National Dose Registry of Canada. Am J Epidemiol. 2001 Feb 15;153(4):309-318.
February 2001
The National Institutes of Health in the United States has published a report from a meeting of experts convened to assess current knowledge in Osteoporosis. Thyroid hormone excess is recognized as a potentially modifiable risk factor for the development of osteoporosis in some individuals. Clearly, patients receiving treatment for thyroid cancer need to have high levels of thyroid hormone to suppress TSH as this has been shown to correlate with survival. In other patients, the optimal levels of thyroid hormone required for treatment of thyroid disease may vary, and should be discussed with your physician. To review the NIH report on Osteoporosis, see Osteoporosis Prevention, Diagnosis, and Therapy When does the thyroid gland enlarge physiologically and what happens during puberty? This issue was examined in Switzerland in 259 healthy adolescents (110 girls and 149 boys), aged 11-17 yr. The growth of the thyroid correlates reasonably well with total body growth, but after girls develop menarche (onset of menstruation), the thyroid growth rate increases. See Sex-Dependent Variations and Timing of Thyroid Growth during Puberty. J Clin Endocrinol Metab. 2001 Feb 1;86(2):750-754.
November 2000
How does radiation increase the incidence of thyroid cancer?
A subset of patients with radiation-induced thyroid cancer exhibit a fusion between two genes, the RET and H4 genes, leading to the ret/PTC oncogene. It now appears that radiation may predispose to the development of this genetic abnormality due to the close anatomical proximity of these two genes in normal thyroid cells, permitting radiation exposure to "hit both genes" at the same time. To review the data, see Proximity of chromosomal loci that participate in radiation-induced rearrangements in human cells Science 2000 Oct 6;290(5489):138-41.
Prevalence of Thyroid disease in a large population in Norway
It is not uncommon for patients to have previously undetected hypothyroidism that may be detected in a large screening program. Review the results in Prevalence of thyroid disease, thyroid dysfunction and thyroid peroxidase antibodies in a large, unselected population. The Health Study of Nord-Trondelag (HUNT). Eur J Endocrinol 2000 Nov;143(5):639-647.
October 2000
Prevalence of Hypothyroidism in women
Consistent with prevailing impressions, hypothyroidism may be more common than previously thought. In a cohort of women over age 50 in Ireland, the prevalence of overt spontaneous primary hypothyroidism was 8.6% in 544 females aged 50 years or more but only 0.9% in the 1,000 females between 18 and 50 years of age. Most of the patients with hypothyroidism had positive thyroid antibodies, consistent with an autoimmune origin of the disease. See Hypothyroidism and aging: the Rosses' survey Thyroid 2000 Sep;10(9):821-7.
September 2000
Mapping a Dominant Form of Multinodular Goiter to Chromosome Xp22
Multinodular goiter (multiple nodules in an enlarged thyroid) often runs in families, and is more common in women than men. An new study of a large Italian family has identified a region of the X chromosome that when inherited increases the risk of developing multinodular goitre in affected female subjects. Although it is not possible to generalize these findings to the individual patient with multiple thyroid nodules, further studies of this type may provide more information about why some individuals develop thyroid nodules, whereas other family members may not. To review the genetic data, see Am J Hum Genet 2000 Oct;67(4):1004-1007.
August 2000
New oncogene identified in human follicular thyroid cancer
The common forms of well differentiated thyroid cancer, papillary and follicular carcinoma, exhibit histological differences and differ somewhat in their behavior. Mutations in the ret oncogene have previously been identified in some patients with papillary thyroid cancer (PTC). A new report identifies an abnormal fusion of 2 proteins, the pax8 transcription factor and the PPARg1 transcription factor, as a potentially important oncogenic abnormality in patients with follicular carcinoma of the thyroid. The Pax8-PPARg1 fusion protein was detected in 5/8 follicular cancers, but not in PTC or in patients with benign thyroid disease. These findings suggest that detection of this protein may aid in the diagnosis of benign vs malignant thyroid tumors, and ultimately, new treatment strategies may be designed to circumvent the activity of the abnormal protein. See Science 289:1357-1360.
Heart surgery in children and T3 replacement
It is well known that many patients with severe illness exhibit alterations in levels of circulating thyroid hormones, a constellation of findings often referred to as the "euthyroid sick syndrome". A new randomized study of 40 children receiving open heart surgery suggests that T3 treatment during the perioperative period may confer some benefit. See Lancet 2000 Aug 12;356(9229):529-34. Although the study is small, it will stimulate additional investigation in this area and a second group has published similar results in 7 infants undergoing open heart surgery. J Thorac Cardiovasc Surg 2000 Sep;120(3):604-608. Studies of thyroid hormone replacement in critically ill adults have frequently been inconclusive with regard to potential benefit.
Breast cancer and radioactive iodine treatment?
At present, radioactive iodine administration is generally reserved for treatment of patients with hyperthyroidism or thyroid cancer. New evidence suggests that lactating breasts and some breast cancers may express a protein similar to the iodine transporter produced in normal and cancerous thyroid cells. These findings suggest that future studies should focus on the possibility that some patients with breast cancer may be candidates for radioactive iodine treatment, if the work is confirmed in larger human studies. See the paper in Nature Medicine 2000 Aug;6(8):871-8 The mammary gland iodide transporter is expressed during lactation and in breast cancer.
IgE and the response to therapy in Hyperthyroidism
The reasons why some patients respond rapidly to treatment with antithyroid drugs and develop sustained remissions, whereas other patients exhibit less optimal responses, remain poorly understood. A study of Japanese patients with Graves' disease suggests that some patients with elevated levels of the immunoglobulin protein IgE appear to respond less favorably and exhibit a lower remission rate during treatment with antithyroid drugs such as methimazole. See An elevation of serum immunoglobulin E provides a new aspect of hyperthyroid Graves' disease. J Clin Endocrinol Metab 2000 Aug;85(8):2775-8.
Management of Solitary Thyroid Nodules
What tests does the average North American or European thyroid endocrinologist routinely recommend in the initial investigation of a patient with a thyroid nodule? The 2 most common tests are 1) a TSH blood test and 2) a fine needle aspiration biopsy. To review the results of this survey, see Management of the solitary thyroid nodule: results of a North American survey J Clin Endocrinol Metab. 2000 Jul;85(7):2493-8.
July 2000
A new study of babies with infantile hemangiomas, an abnormal proliferation of blood vessels, demonstrates that these hemangiomas may cause hypothyroidism in affected infants. Some of the hemangiomas appear to express an enzyme, type 3 iodothyronine deiodinase, that rapidly inactivates thyroxine in the blood, leading to hypothyroidism if the thyroid cannot keep increase production of thyroid hormone to match the increased rate of degradation. Review the original study in Severe Hypothyroidism Caused by Type 3 Iodothyronine Deiodinase in Infantile Hemangiomas. N Engl J Med. 2000 Jul 20;343(3):185-189.
June 2000
May 2000
New data on outpatient use of radioactive iodine and exposure in the home environment Radiation exposure from outpatient radioactive iodine (131I) therapy for thyroid carcinoma. JAMA. 2000 May 3;283(17):2272-4.
April 2000
The incidence, prevalence and mortality statistics are now available for all types of cancers via the Canadian Cancer Society Cancer Statistics 2000 database. These data do show a significant increase in the number of reported cases of thyroid cancer in both men and women. Importantly, as noted in the report summary, the mortality rate for thyroid cancer is not increasing, nor is it expected to do so, given the excellent treatment results achieved in the majority of patients. For hard data on the excellent survival statistics, note that the mortality rate for thyroid cancer cases is essentially lower than that for all other cancers studied by this registry, as shown in Table 1, Estimated New Cases and Deaths for Cancer Sites and Gender, 2000.
February 2000
The Colorado Thyroid Disease Prevalence Study
Thyroid dysfunction may be more common than previously appreciated. In a study of 25,862 patients attending a state health fair, the prevalence of elevated TSH determinations was ~ 9.5% and ~2% of patients had a low TSH. Surprisingly, among patients on L-thyroxine with known thyroid disease, 40% had abnormal TSH determinations. To view a Summary of the Study, or the entire publication, see The Colorado Thyroid Disease Prevalence Study Archives of Internal Medicine 2000:160;526-534.
February 2000
Hypothyroidism and Heart Disease in Women
The Annals of Internal Medicine reports a study describing an increased prevalence of subclinical hypothyroidism in women with aortic atherosclerosis and myocardial infarction. The study does not prove cause and effect, nor does it infer that treatment of hypothyroidism will modify the development of the diseases. For the original report, see Subclinical Hypothyroidism Is an Independent Risk Factor for Atherosclerosis and Myocardial Infarction in Elderly Women: The Rotterdam Study Annals of Internal Medicine, 15 February 2000: 132:270-278. For an overview of the article, see the Non-technical Summary.
December 1999
Tipper Gore had a hemi-thyroidectomy for a thyroid nodule December 28, prompting extensive media coverage of thyroid nodules, biopsies, and thyroid cancer.
November 1999
The FDA has issued a warning regarding the use of a dietary supplement known as "Triax Metabolic Accelerator". This supplemented is marketed for weight loss by Syntrax Innovations Inc in the United States. According to the FDA, this product may produce clinical hyperthyroidism as it contains tiratricol (also known as TRIAC or 3,5,3'-triiodothyroacetic acid), a molecule that functions as a thyroid hormone analog. The FDA issued its warning following the development of severe clinical hyperthyroidism in a husband and wife couple from California. To review the effects of tiratricol in a well-designed clinical study, see J Clin Endocrinol Metab 1997 Jul;82(7):2153-8 Augmented hepatic and skeletal thyromimetic effects of tiratricol in comparison with levothyroxine.
New Data on the long term follow-up of patients with hyperparathyroidism from the New England Journal of Medicine. See the Parathyroid Glands Section for an overview.
August 1999
Maternal thyroid function during pregnancy and neuropsychological development of the child.
In the Aug 1999 issue of the New England Journal of Medicine, a new study reports the results of neuropsychological testing (IQ tests, school performance, language and reading skills, visual and motor performance) in 62 women with varying degrees of hypothyroidism during pregnancy. There was a small but significant difference in IQ scores in children whose mothers were not treated for their hypothyroidism during pregnancy.
These results reaffirm the importance of maintaining thyroid function at a normal level in woman planning a pregnancy, and in pregnant women. As thyroid hormone requirements commonly increase during pregnancy, pregnant women taking thyroid hormone should be appropriately monitored to make sure their TSH remains in the normal range.
